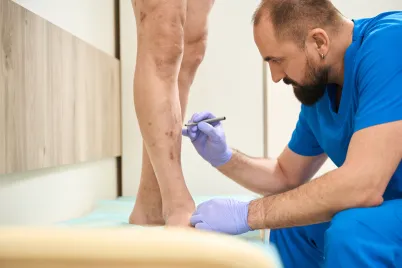
Varicose veins are a common condition that affects many adults, presenting as swollen, twisted veins that are visible just under the surface of the skin. While often seen as a cosmetic issue, they can also cause discomfort and may indicate underlying circulatory problems. Understanding the nature of varicose veins, their symptoms, and the available management options is a step toward addressing the condition and enhancing overall well-being.
What Are Varicose Veins?
Varicose veins are enlarged, gnarled veins that most often appear on the legs and feet. They occur when the valves within the veins become weak or damaged. These valves are responsible for preventing blood from flowing backward. When they do not function properly, blood can pool in the veins, causing them to stretch and swell. Several factors can increase the likelihood of developing varicose veins. These include genetics, age, gender, pregnancy, and prolonged periods of standing.
What Are the Symptoms?
The signs and symptoms can vary among individuals. The most recognizable sign is the appearance of dark purple or blue veins that are twisted and bulging, resembling cords on the legs. In addition to their appearance, they can also lead to physical discomfort. Common symptoms include:
- An achy or heavy feeling in the legs
- Burning, throbbing, muscle cramping, and swelling in the lower legs
- Pain that worsens after sitting or standing for a long time
- Itching around one or more of the veins
In some cases, more serious complications can arise, such as skin discoloration, ulcers near the ankle, or blood clots. Recognizing these symptoms early can help in managing the condition effectively.
What Treatments Work Best?
A range of treatment options is available, from self-care measures to medical procedures. The appropriate course of action depends on the severity of the symptoms and individual health factors. For many, lifestyle adjustments such as exercise, leg elevation, and wearing compression stockings can help alleviate pain and prevent the condition from worsening.
When conservative measures are insufficient, a healthcare provider may recommend more advanced treatments. Options such as sclerotherapy, laser treatments, and radiofrequency ablation are minimally invasive procedures designed to close off or remove the affected veins. In more severe cases, surgical procedures like vein stripping may be recommended to remove them.
How Can You Prevent Them?
While it may not be possible to prevent varicose veins completely, certain lifestyle changes can reduce your risk and slow their progression. Improving circulation and muscle tone can have a significant impact on vein health. Regular exercise, such as walking or swimming, helps promote healthy blood flow in the legs. Maintaining a healthy weight reduces pressure on the veins, and a high-fiber, low-salt diet can help prevent swelling. Avoiding prolonged periods of sitting or standing and elevating your legs when resting can help improve circulation.
Take Control of Varicose Veins
Managing varicose veins begins with understanding the condition and exploring the most suitable options for your specific situation. Options range from simple lifestyle changes to advanced medical procedures. There are effective ways to reduce symptoms and improve your quality of life. Taking proactive steps and consulting a healthcare professional can help you find the right management plan. If you are experiencing discomfort or are worried about the appearance of your veins, schedule a consultation with a specialist to discuss treatment options.